Postoperative adhesions are among the most common yet underestimated complications in gynecological surgery. They can lead to chronic pelvic pain, infertility, bowel obstruction, and a significant reduction in patients’ quality of life. For this reason, effective adhesion prevention has become a key element of modern, patient-centered gynecological surgery.
Why Adhesion Prevention Is Essential
Surgical trauma, bleeding, and inflammatory responses following pelvic procedures create an environment that promotes the formation of fibrous adhesions between organs and surrounding tissues. Clinical data indicate that a substantial proportion of re-operations in gynecology are directly related to adhesion-associated complications.
Modern Strategies for Adhesion Prevention
Successful adhesion prevention is based on a multimodal approach, including:
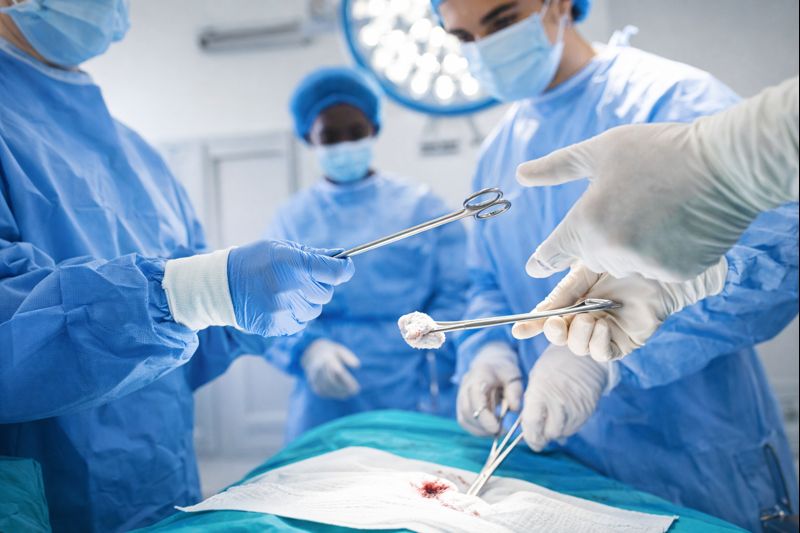
Atraumatic surgical techniques, preferably minimally invasive and laparoscopic
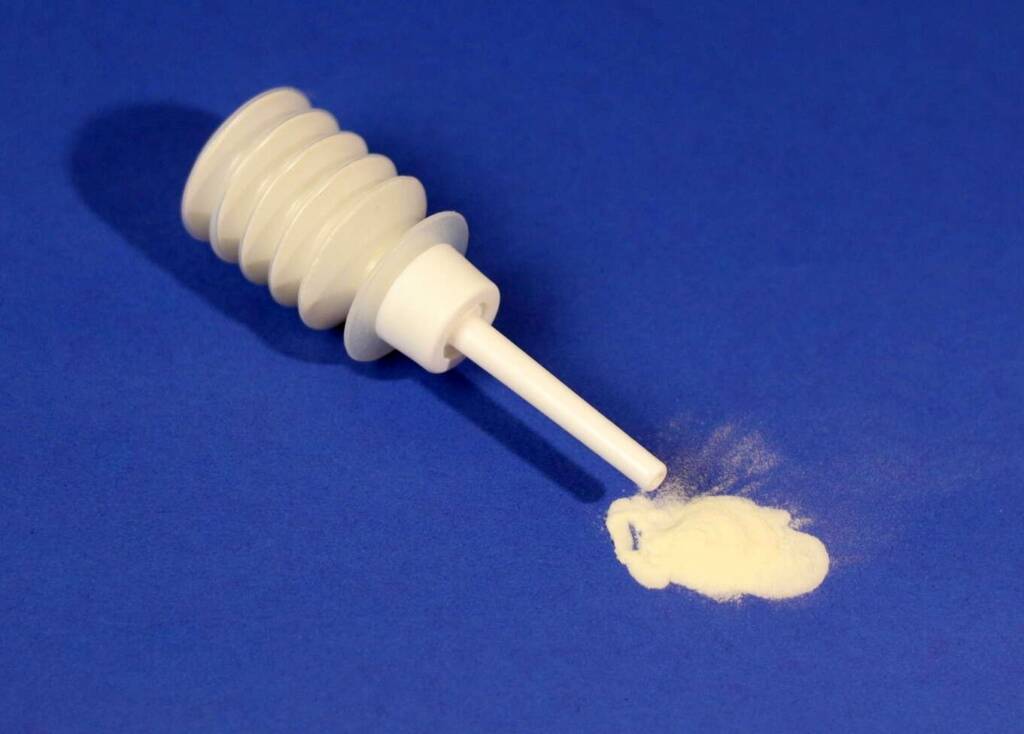
Meticulous hemostasis to avoid residual blood in the surgical field
Minimization of foreign materials
Targeted use of anti-adhesion barriers, such as gels or membranes
In particular, resorbable barrier products can effectively separate vulnerable tissue surfaces during the critical healing phase, thereby reducing the risk of postoperative adhesion formation.
Clinical Relevance in Gynecological Surgery
Daily clinical practice demonstrates that a structured adhesion prevention strategy not only lowers postoperative complication rates but also:
reduces the need for re-operations,
improves patient outcomes and satisfaction,
and contributes to long-term cost efficiency within healthcare systems.
Conclusion
Adhesion prevention should not be considered an optional measure but an integral component of modern gynecological surgery. By combining surgical expertise, precise hemostatic control, and innovative prevention solutions, the risk of postoperative adhesions can be significantly reduced.